This article covers
What are red blood cells – an overview
Red blood cells (RBCs, also called erythrocytes) are the most abundant blood cells. Their function is to carry oxygen from the lungs to all parts of the body.
In this article, you will learn the biology and functions of red blood cells. We will discuss why red blood cells carry oxygen molecules so efficiently and where red blood cells are born in our bodies. I will also show you how they look like under the microscope. Let’s get started.

The components of our circulation system
Before we study the function of red blood cells, we quickly review what the circulation system (or circulatory system) is. For complicated multicellular organisms, efficiently delivering oxygen and nutrients to every cell is a crucial task. In our body, the circulation system takes over this critical job.
In brief, the circulation system transport nutrients and oxygen to and from the cells in the body to provide nourishment. It also helps fight diseases, stabilizes body temperature, and maintain homeostasis (meaning the steady balance of physical and chemical conditions in our body).
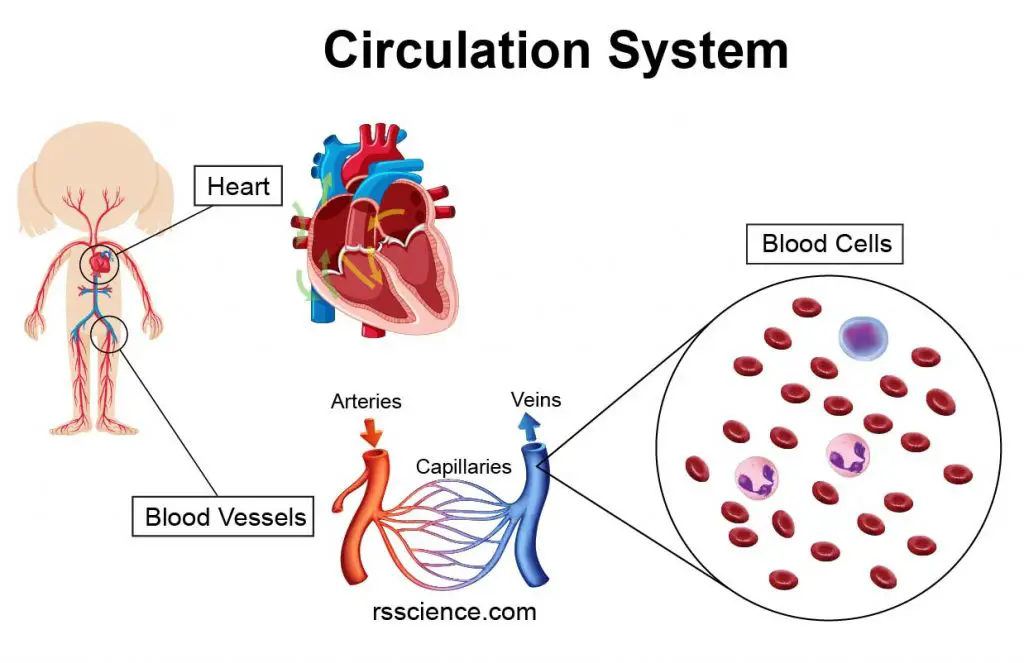
[In this image] The major components of our circulation system include the heart (pump), blood vessels (pipes), and various blood cells (carriers).
The essential components of the circulation system include the heart, blood, and blood vessels. The heart pumps oxygenated blood to the body and recycles deoxygenated blood to the lungs. Blood is carried through the body via blood vessels.
The composition of human blood
Blood is a body fluid that transports nutrients, oxygen, and metabolic waste in our bodies. The average adult has a blood volume of roughly 5 liters.
Blood is composed of blood cells suspended in blood plasma. Plasma, a yellowish fluid, is mostly water and contains various proteins, blood sugar, ions, and carbon dioxide.
The blood cells are mainly red blood cells (also called RBCs or erythrocytes), white blood cells (also called WBCs or leukocytes), and platelets. The red blood cells constitute about 45% of whole blood volume, the plasma about 54%, and white cells about 1%.
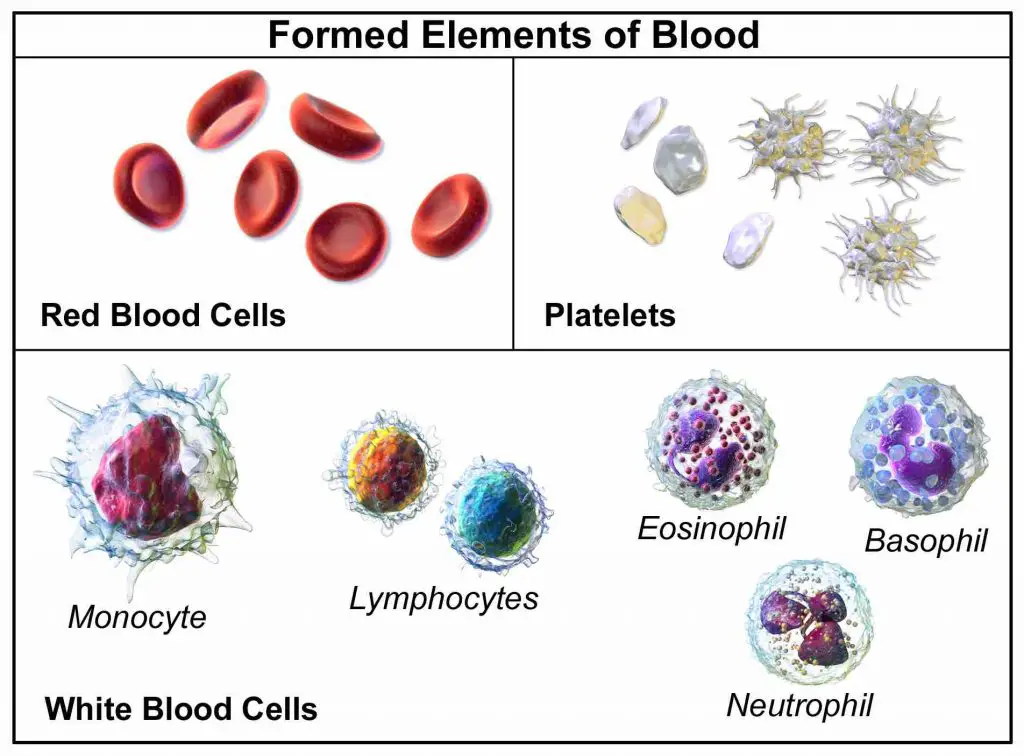
[In this image] The three major types of blood cells – red blood cells, white blood cells, and platelets.
Photo credit: Encyclopedia
What the hematocrit means?
To know the composition of a blood specimen, you can spin a test tube of blood in a centrifugation machine to separate the blood into three fractions.
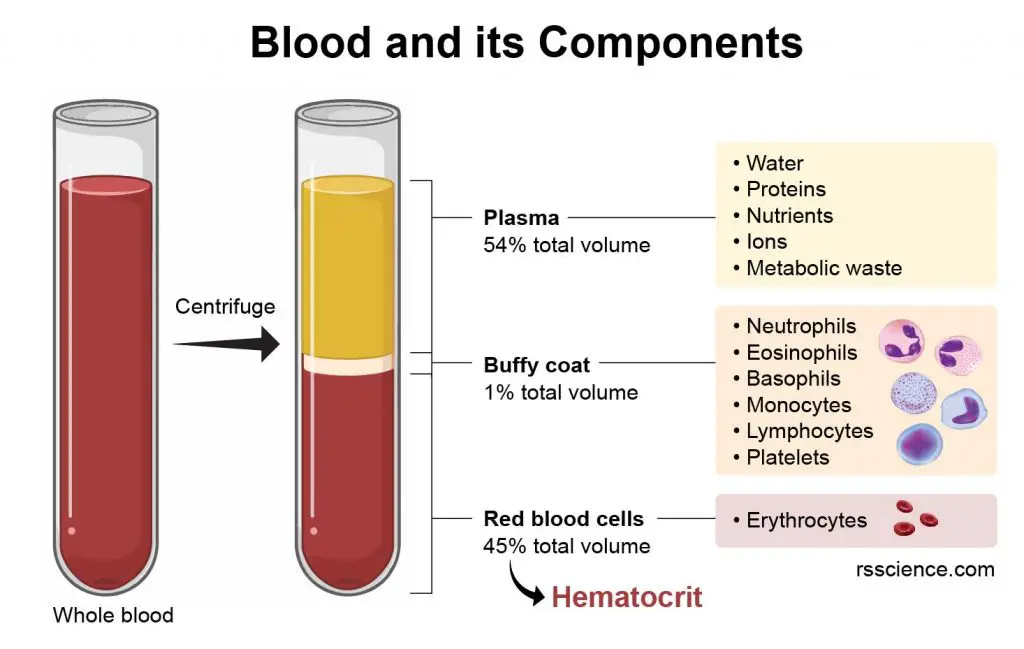
[In this image] Blood contains plasma and blood cells.
Their relative amounts can be measured by the packed volume after the centrifugation. Plasma is lighter, so it floats on the top. Red blood cells are denser, so they are span down to the bottom. Between the plasma and RBCs is a thin layer of the white stuff, called Buffy coat. Buffy coat contains a mixture of various white blood cells.
The volume percentage of red blood cells is referred to as hematocrit (hct), which is measured routinely in blood tests.
Generally, a normal range is considered to be:
- For men, 38.3 to 48.6 percent
- For women, 35.5 to 44.9 percent
- For Newborn, 55 to 68 percent
A low hematocrit could indicate a diseased condition. For example, anemia happens due to an insufficient supply of healthy red blood cells.
What do red blood cells do?
RBCs make up approximately 45% of the total blood volume in a healthy adult, making them the most abundant type of blood cells. We need so many RBCs because they play such a simple but crucial role – oxygen transportation.
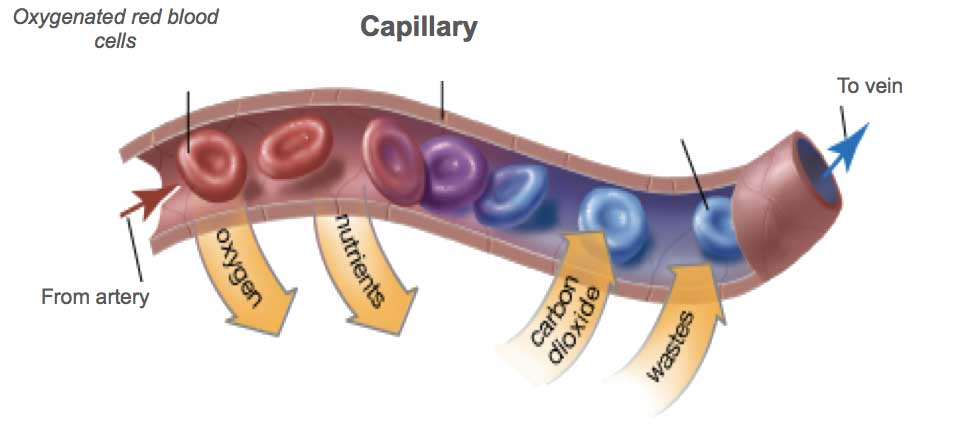
[In this image] Red blood cells carry fresh oxygen all over the body.
Red blood cells take up oxygen in the lungs, or gills of fish, and release it into tissues while squeezing through the body’s capillaries (tiniest blood vessels with close proximity to cells). The distance of oxygen to diffuse in tissues is less than 200 µm. For this reason, the networks of capillaries must cover every inch of our bodies.
[In this video] Red blood cells flow in blood vessels.
Red blood cells at work
Size, Color, and Lifespan
Mature human RBCs look like oval biconcave disks. They are about 7.5 µm in diameter and 2 µm in thickness. The red color is due to the presence of iron in hemoglobin, the most abundant oxygen-carrying protein in RBCs.
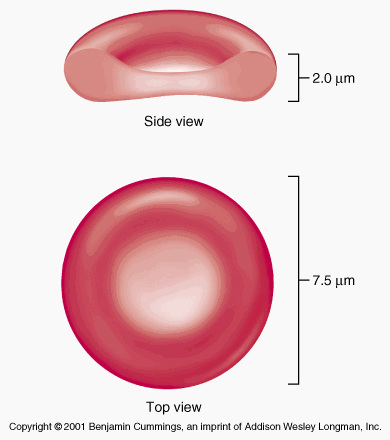
[In this image] Human red blood cell appears dumbbell-shaped in profile.
Photo credit: Socratic Q&A
Oxygenated blood (fresh pumped out from the heart) is bright red, and deoxygenated blood (returning to the heart from the body) is dark red. Adults have roughly 20 – 30 trillion RBCs at any given time. Approximately 2 million new RBCs are produced per second in the bone marrow and circulate for about 120 days in the body.

[In this image] Two drops of blood are shown with a bright red oxygenated drop on the left and a deoxygenated drop on the right.
Photo credit: wiki
Unique cell structure
No nucleus
Human (and mammalian) RBCs lack cell nuclei and most organelles to accommodate maximum space for hemoglobin and keep flexible, so it is easy for them to squeeze through capillaries. The elimination of the nucleus happens during the maturation of RBCs from their progenitor cells.
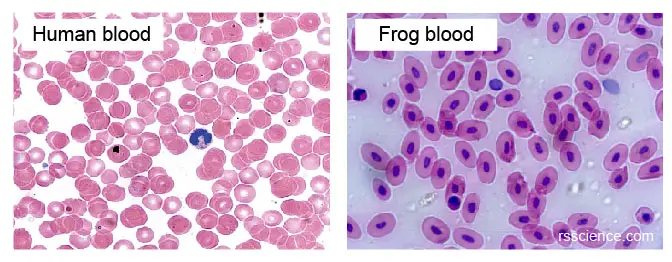
[In this image] Mammalian RBCs don’t have cell nuclei. However, other vertebrates, such as fish, frogs, or birds, all keep the nuclei in their RBCs. Mammalian RBCs are also smaller than others.
Flexible cell membrane
The cell membrane plays a major role in keeping RBCs deformable, flexible, and stable. The red blood cell membrane is composed of 3 layers:
(1) The glycocalyx on the exterior, which is rich in carbohydrates.
(2) The lipid bilayer, which contains many transmembrane proteins
(3) The membrane skeleton, a structural network of proteins located on the inner surface of the lipid bilayer.
Total proteins can contribute to as high as 50% of the RBC membrane mass. The other half are lipids, namely phospholipids and cholesterol.
The ABO blood types are due to variations in surface glycoproteins of red blood cells.
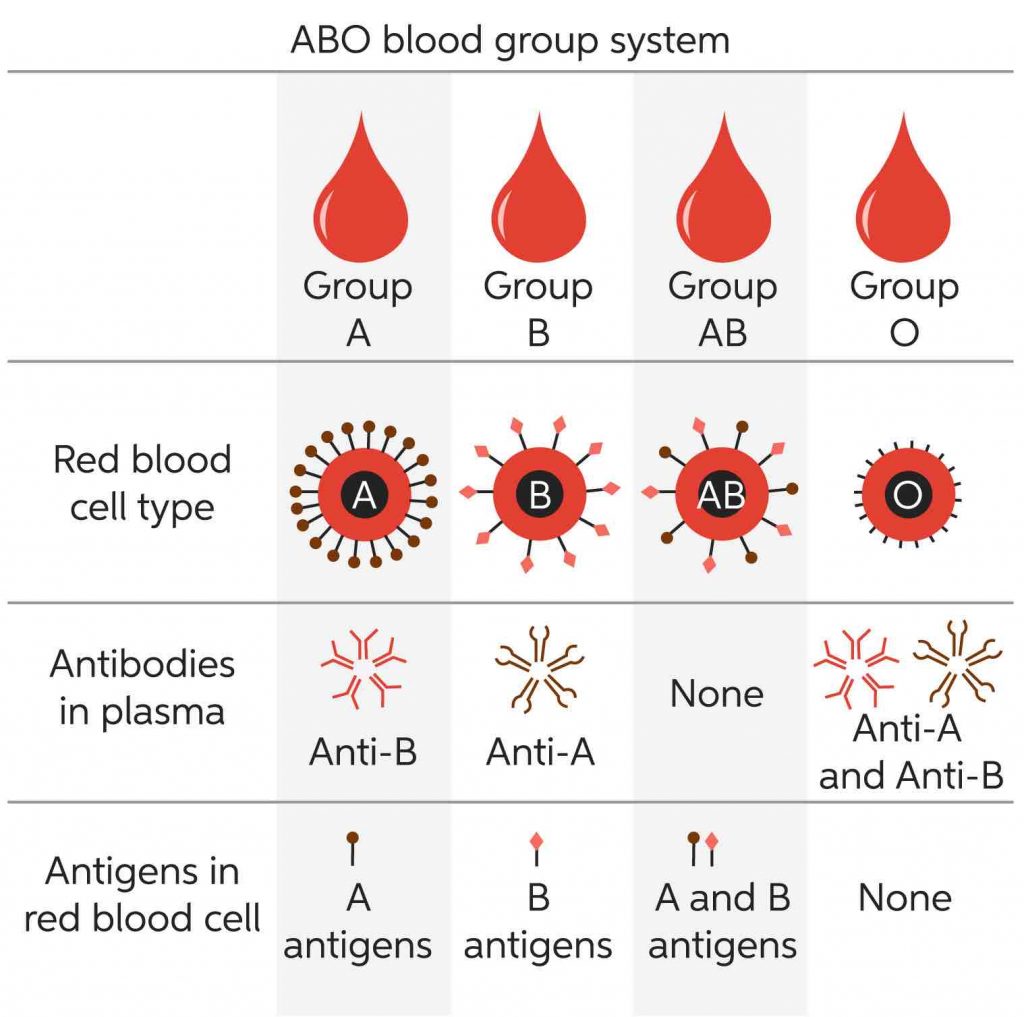
[In this image] ABO blood group system.
Photo credit: Chegg
Hemoglobin
The cytoplasm of RBCs is rich in hemoglobin (Hb), an iron-containing protein complex that can bind oxygen. Each human red blood cell contains approximately 270 million of these hemoglobin molecules.
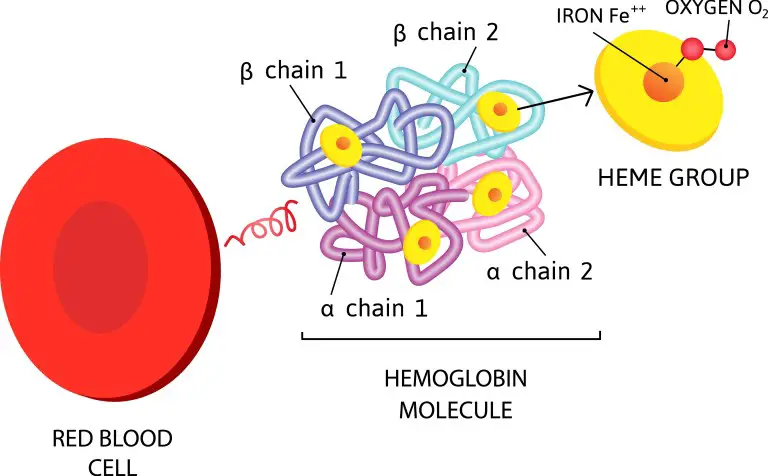
[In this image] A hemoglobin is formed by four globulin chains. Each globulin carries a heme, which contains an iron atom. These iron atoms are the center of oxygen binding.
Hemoglobin is made up of four protein units (globulin chains) that are connected together. The adult hemoglobin molecule contains two alpha-globulin chains and two beta-globulin chains. In fetuses and infants, their hemoglobin molecule is made up of two alpha chains and two gamma chains. As the infant grows, the gamma chains are gradually replaced by beta chains.
Each globulin chain contains an important iron-containing porphyrin compound, called heme. Embedded within the heme compound is an iron atom that is vital in transporting oxygen and carbon dioxide in our blood. The iron in hemoglobin is also responsible for the red color of blood.
The beauty of hemoglobin is that it can bind to oxygen with a strong affinity in the lung or gill (where the oxygen level is high). When hemoglobin travels to tissues (where the oxygen level is low), its structure changes, and the affinity between heme and oxygen decreases, releasing its oxygen cargo.
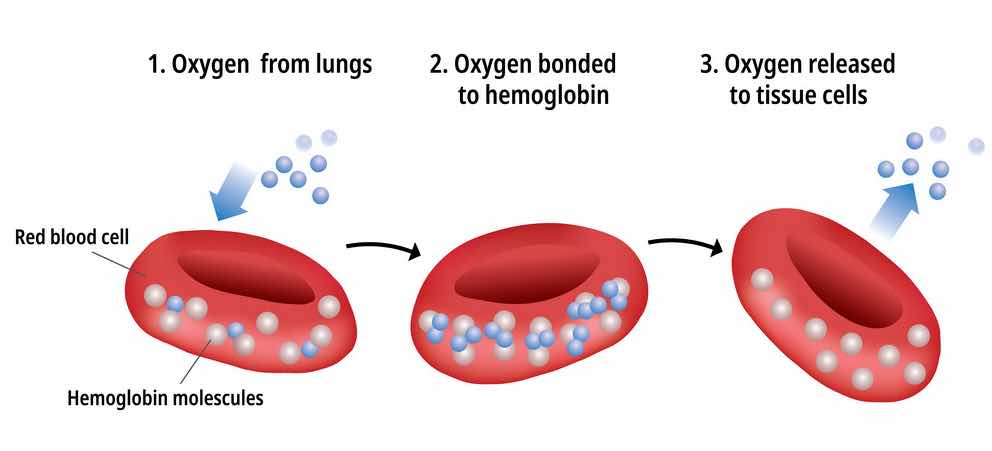
[In this image] Hemoglobin mediates the oxygen transportation between the lung and other tissues.
Hemoglobin also plays an important role in maintaining the shape of the red blood cells. Abnormal hemoglobin structure can, therefore, disrupt the shape of red blood cells and impede their function (i.e., sickle cell anemia).
Life cycle of red blood cells
Human red blood cells are produced in the bone marrow (in the liver for infants).
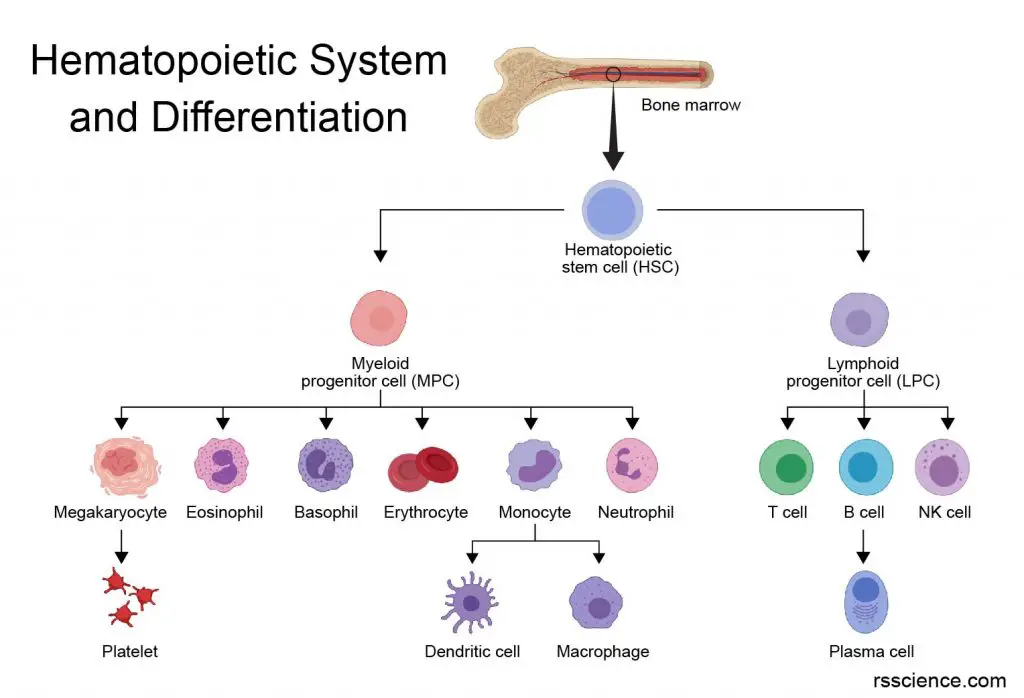
[In this image] The family of the hematopoietic (meaning blood) system originates from the hematopoietic stem cells in our bone marrow.
We have the most potent blood-forming stem cells, called hematopoietic stem cells (HSCs), that reside in the bone marrow. HSCs can divide and differentiate into erythroblasts, which are committed progenitors of RBCs. By a process called erythropoiesis (talks 7 days), erythroblast gradually fills with hemoglobin, and its nucleus and mitochondria disappear, becoming reticulocytes. Reticulocytes ultimately become fully mature red blood cells. The average red blood cells in humans can live for 100-120 days.
Erythropoiesis can be stimulated by a hormone called erythropoietin (EPO), which is synthesized by the kidney. EPO can be given as a drug to treat anemia (low RBC condition). In fact, recombinant human erythropoietin (rhEPO) was the first protein drug produced through recombinant DNA technology by Amgen in 1989.
High hematocrits can be seen in people living at high altitudes. Elite marathon runners may obtain training at high altitudes to improve their blood oxygen efficiency. However, some athletes may abuse the drug erythropoietin for “blood doping” purposes.
Look at red blood cells under a microscope
Preparation and staining of blood smear
There are over 5 million red blood cells per cubic millimeter of blood. If you just add a drop of blood on a microscopic slide, the specimen will be too “thick” (too many cells) to observe.
For this reason, making a diluted specimen is generally required. The most common way is to prepare a “Blood Smear” and then stain with Wright-Giemsa solution. You can check out “White blood cell post” to learn how to make a blood smear.
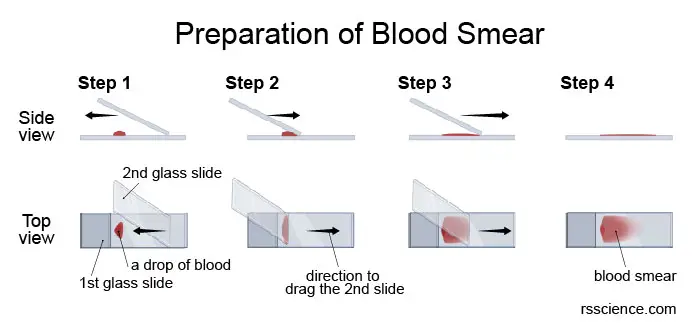
[In this image] Microscopic examination of whole blood begins with the preparation of a smear.
Blood cells under the microscope
If the blood film is properly prepared and stained, we should easily see individual cells under a bright-field microscope. You should see RBCs everywhere as they are the most abundant cells in the blood. Notice that human RBCs don’t have nuclei and look like a dish. You can also see several types of white blood cells (WBCs) at a much lower frequency. Click here if you would like to know how to identify different WBCs.
Note: Without staining, the RBCs don’t look “red” under the microscope. The pink-red color in the image below comes from the eosin dye of Wright-Giemsa stains.
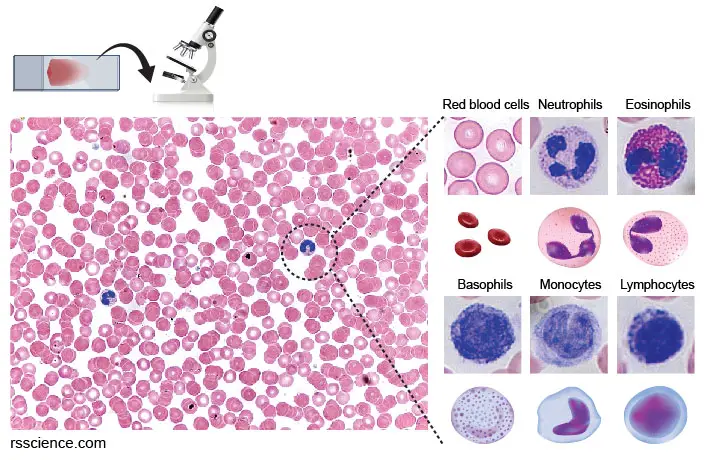
[In this image] After preparing blood smear and Wright-Giemsa staining, you can look at these blood cells under a bright-field microscope. The blue color comes from the Methylene blue dye, which stains the DNA in nuclei. These pink-red oval disks without nuclei are RBCs.
Note that the cell structure of RBCs is generally unsubstantial than that of WBCs. For example, RBCs can burst easily in an RBC lysis buffer containing ammonium chloride (a hypotonic solution). However, WBCs have minimal effect in this solution. Don’t add pure water to your blood sample because it will generate the same lysis outcome. Use a saline solution if you need to dilute a blood specimen.
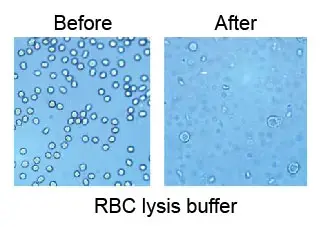
[In this image] After being treated with RBC lysis buffer, all RBCs disappear.
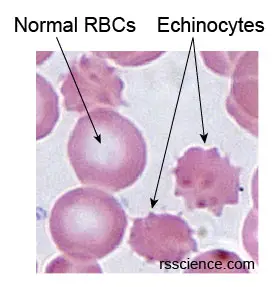
[In this image] The star-shaped echinocytes are a result of an artifact usually found in old samples.
Diseases related to red blood cells
Problems with red blood cells can be due to illnesses or a lack of iron or vitamins in the diet. Some diseases of the red blood cells are inherited.
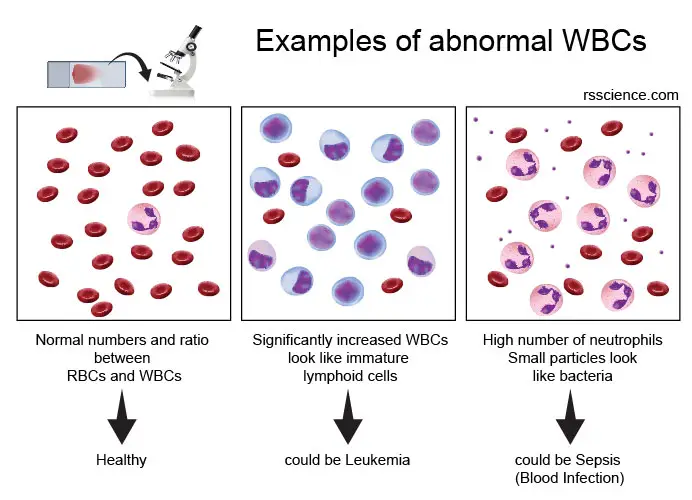
[In this image] Two examples of diseases associated with abnormal RBCs. An experienced hematologist can have a clue of what is wrong in your body by examining your blood cells by the complete blood count (CBC) or blood smear.
Anemia
A person who has a low hematocrit is referred to as being anemic. There are many reasons for anemia. Some of the more common reasons are:
- loss of blood (traumatic injury, surgery, bleeding, and colon cancer)
- nutritional deficiency (iron, vitamin B12, folate),
- bone marrow problems (replacement of bone marrow by cancer, suppression by chemotherapy drugs, kidney failure)
- abnormal hemoglobin (sickle cell anemia).
Sickle cell anemia
Sickle cell disease (SCD) is an inherited disorder. It happens because of a mutation in the hemoglobin gene. The abnormal hemoglobin causes red blood cells to become rigid, sticky, and unable to flow smoothly through blood vessels. Sickle cells die much faster than normal RBCs – in 10 to 20 days instead of 120 days. This causes a shortage of red blood cells.
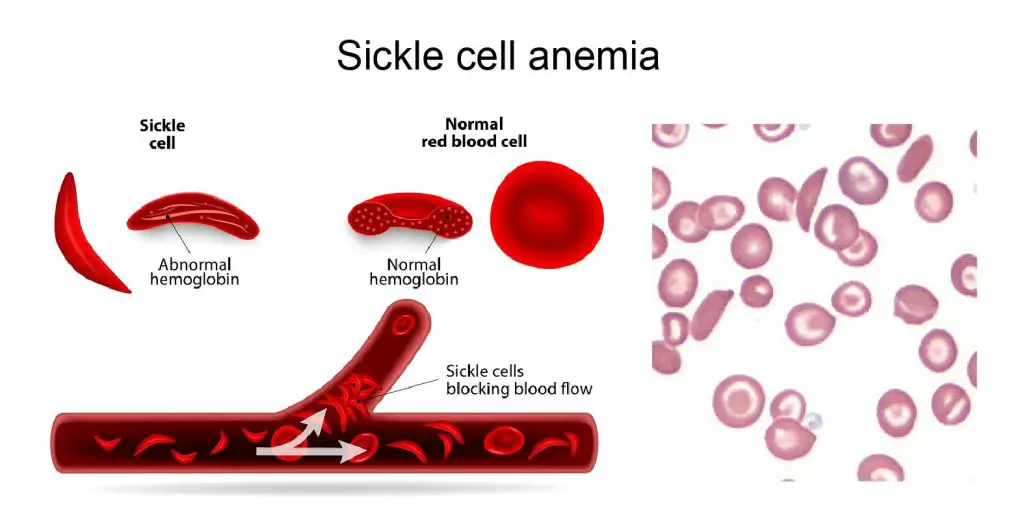
[In this image] Sickle cell anemia is caused by abnormal hemoglobin. In this inherited disease, the red blood cells are shaped like half-moons rather than the normal indented circles. Right: the actual image of sickle cells.
Photo credit: Science
Sickle cell disease affects millions of people in many developing countries. A blood and bone marrow transplant is currently the only cure for sickle cell disease, but only a small number of patients are eligible. You would expect natural selection to weed out a gene that has such unpleasant consequences, but with sickle cell disease, that doesn’t seem to be the case. Indeed, the cases of sickle cell stay sustained in the human population.
One explanation is that sickle cell disease had developed a wired relation with another disease – Malaria. Malaria is a mosquito-borne disease caused by a parasite. This parasite, Plasmodium falciparum, invades, feeds, and grows inside the RBCs. People with only one sickle cell gene (called sickle cell trait) didn’t cause discomfort by Sickle cell disease but are protected from severe forms of malaria. The protection from malaria could be the driving force to maintain sickle-cell traits in the human population.
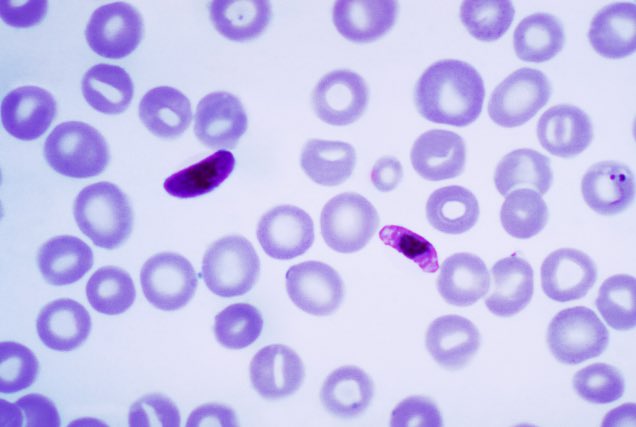
[In this image] A blood smear showing the infection of Plasmodium falciparum parasites.
Photo credit: wiki